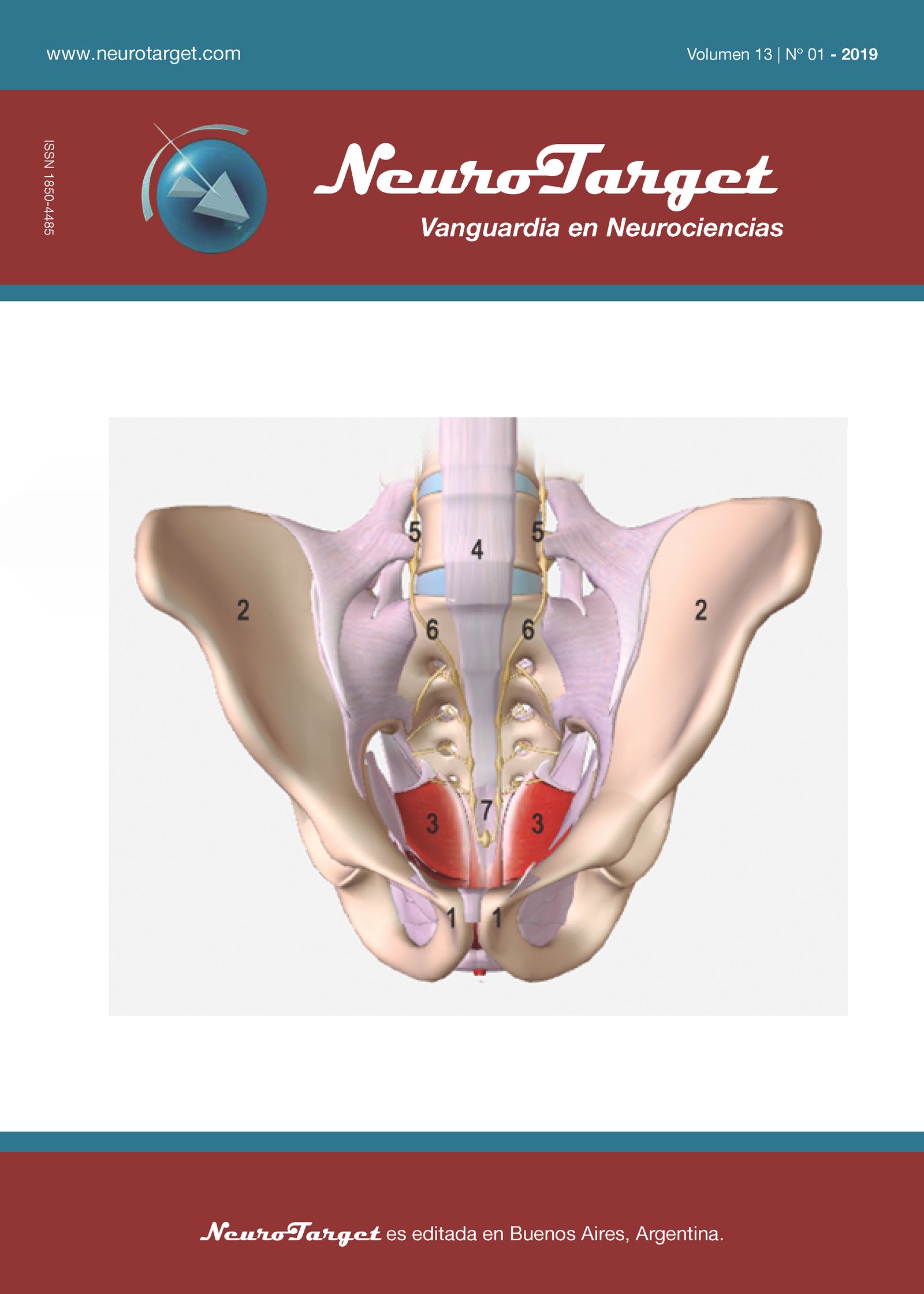
Anatomical study of the ganglion impar
DOI:
https://doi.org/10.47924/neurotarget201936Keywords:
ganglion impar, block, sacrococcygeal joint, interureteral lamina, presacral fasciaAbstract
Introduction: The sacral laterovertebral portions of the sympathetic chains (CSLS) are joined by an anastomotic loop anterior to the sacrococcygeal joint or to the first coccygeal vertebra. This results in the formation of the Ganglion Impar (GI). This one receives nociceptive projections and the sympathetic innervation of the distal viscera of the pelvis and perineum, being a target of nervous blockade for painful pathologies of the region.
Purpose: To study the frequency of formation, morphology, location and relations of the GI and thus provide the outfit that enables to approach the area with security.
Materials and methods: Thirty-seven cadaveric pelvic preparations were used, one of them sagittally sectioned, exclusively forphotographic mostration. The instruments used were: left handclamp, Metzenbaum and Iris scissors, handles and scalpel blades. Due to the deep location of the estructures, 3D photographs were taken.
Results Prevalence and location: The GI was found in 66.67% of the cases (24/36). Of these, in 50% (12/24) standing anterior to the transverse line between the fourth and fifth sacral vertebrae (high formation); and in 50% (12/24) at the level of the sacrococcygeal joint (low formation). Relations: The CSLS is deep to the interureteral lamina, to the presacral fascia and to the proximal attachments of the piriformis muscle (anterior to posterior). In the absence of GI, the nervous fillets pass between thea pex of the coccyx and the levator ani muscle, being related to the lateral sacral vessels.If it is presented, the GI rests on the middle sacral vessels, both of which are contained in separate sheaths. Relationship: The relationships differ according to the training height. Morphology of the GI. Of the total cases, 29.17% presented a rectangular shape, 12.5% triangular, and 58.33% plexiform. Approaches: The approaches were performed at the level of the midline, these being: transsacrococcygeal, intercoccygeal and anococcygeal.
Conclusion: We conclude that the formation of the ganglion is prevalent, and the predominant morphology is the plexiform. It should be remarked that all the elements of the presacrococcygeal region lie behind the presacral fascia. We consider that the safest approach is through the transsacrococcygeal joint.vThe knowledge of the anatomy and the relationships of the GI is extremely important to make approaches to it.
Metrics
References
Pró E. Anatomía clínica. 1° Edición. Buenos Aires: Médica Panamericana; 2012: 697.
Rouviere H, Delmas A. Anatomía humana: descriptiva, topográfica y funcional. Tomo 2: Tronco. 11° Edición. Barcelona: Editorial Elsevier Masson; 2005: 294-295.
Testut L, Latarjet A. Tratado de anatomía humana. Tomo tercero: Meninges – Sistema nervioso periférico - Órganos de los sentidos - Aparato de la respiración y de la fonación - Glándulas de secreción interna. 9° Edición. Barcelona: Editorial Salvat Editores; 422-424.
Ganduz O. H., Sencan S., Kenis-Coskun, O. Pain Relief due to Transsacrococcygeal Ganglion Impar Block in Chronic Coccygodynia: A pilot Study.
Gürses E. Impar ganglion radiofrequency application in successful management of oncologic perineal pain.
Albanese, A. R. La lámina interureteral.
Agarwal Kozlowski K., Lorke D. E., Habermann C. R., Beck H. CT-guided blocks and neuroablation of the Ganglion Impar (Walther) in perineal pain: Anatomy, technique, safety and efficacy.
Cortiñas M., Muñoz Martín T., Vara C., Salmeron J., García Villarba F. Eficacia del bloqueo del ganglio impar en dolor pélvico y perineal de etiología ginecológica rebelde al tratamiento médico-quirúrgico.
Pérez Rosillo M. A., Guzman Álvarez L., Castellano García, M. D. M., Molina Martín A. A., Revelles Paniza M., Ruiz Santiago F. ¿Ganglio Impar?: Bloqueo nervioso guiado por TCMC en el tratamiento del dolor perineal y coccígeo.
Restrepo Garces, C.E., Gómez Bermúdez, C.M., Jaramillo Escobar, S., Ramírez, L. J., Vargas, J.F. Procedimientos a nivel del ganglio impar.
Oh C. S., Chung I. H., Ji H. J., Yoon D. M. Clinical implications of topographic anatomy on the Ganglion Impar.
Fawcett M. B. An unusual mode and site of termination of the right sacral sympathetic cord.
Walters A., Muhleman M., Osiro S., Bubb K., Snosek M., Shoja M. M., Tubbs R. S., Loukas M. One is the loneliest number: A review of the Ganglion Impar and its relation to pelvic pain syndromes.
Marker D. R, U-Thainual P., Ungi T., Flammang A. J., Fichtinger G., Iordachita I. I., Carrino J. A., Fritz J. MR-guided perineural injection of the ganglion impar: technical considerations and feasibility.
Rigaud J., Delavierre D., Sibert L., Labat J. J. Les infiltrations du système nerveux sympathique dans la prise en charge thérapeutiques des douleurs pelvipérinéales chroniques.
Cardaillac C., Ploteau S., Labat J. J., Levesque A., Riant T. Intérêt de l’infiltration du ganglion Impar dans les vulvodynies rebelles: à propos d’une série de 8 casInterest of infiltration of Impar node in rebel vulvodynia: About a series of 8 cases.
Datir A., Connell D. CT-guided injection for ganglion impar blockade: a radiological approach to the management of coccydynia.
Malec Milewska M., Horosz B., Koleda I., Sekowska A., Kucia H., Kosson D., Jakiel G. Neurolytic block of ganglion of Walther for the management of chronic pelvic pain.
Scott Warren J. T., Hill V., Rajasekaran A. Ganglion Impar blockade. A review.
Gopal H., Mc Crory C. Coccygodynia treated by pulsed radio frequency treatment to the Ganglion of Impar: A case of series.
Loev M. A., Varklet V. L., Wilsey B. L., Ferrante F. M. Cryoablation: A novel approach to neurolysis of the Ganglion Impar.
Young D. C., Chun W. Y., Jung U. H., Jang H. S., Won J. N., Sora O., Byung-Gun, K. Transsacrococcygeal approach to the ganglion impar block for treatment of chronic coccygodynia after spinal arachnoid cyst removal.
Day M. Sympathetic Blocks: The evidence.
Plancarte Sánchez R., Guajardo Rosas J., Guillen Nuñez R. Superior Hypogastric plexus block and ganglion impar (Walther).
Wemm Jr K, Saberski L. Modified approach to block the ganglion impar (ganglion of Walther.). Reg Anesth. 1995;20:544–5.
Munir MA, Zhang J, Ahmad M. A modified needle-insideneedle technique for the ganglion impar block. Can J Anesth. 2004;51:915–7
Foye PM. New approaches to ganglion impar blocks via coccygeal joints. Reg Anesth Pain Med. 2007;32:269.
Hong JH, Jang HS. Block of the ganglion impar using a coccygeal joint approach. Reg Anesth Pain Med. 2006;31:583–4. 14.
Huang JJ. Another modified approach to the ganglion of Walther block (ganglion of impar). J Clin Anesth. 2003;15:282–3
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2019 Julieta Paredes, Rafael Gigena, Adriana Iacarino, Sofía Castro, Carolina Ibañez, Joaquín Chuang, Sergio Shinzato, Vicente Hugo Bertone, Esteban Blasi

This work is licensed under a Creative Commons Attribution 4.0 International License.
The article is distributed under the Creative Commons Attribution 4.0 License. Unless otherwise stated, associated published material is distributed under the same licence.